Members of a Certain Age
and the Health Plan Consumer Experience

Tracking the Trends in Health Insurance CX
With 2022 data hot off the press, this report gives the industry two years of CX perspectives and the ability to start looking at emerging trends in a time of rapid digital acceleration. In 2021, Zipari, together with partner Ipsos, launched an inaugural consumer experience survey to gather current and direct feedback from health plan members and health plan leaders.
Overall, we saw high rates of member satisfaction in an industry known for lagging behind, and we saw consistent factors predicting this satisfaction. Plans who were able to personalize the health insurance experience and allow their members to send and receive health plan communication only via preferred channels were the plans with the satisfied members.
Digital CX platforms are, of course, the foundation that enables both personalization and omnichannel communication, so it was no surprise that digital tools were associated with both members’ ratings of satisfaction and payers’ report of positive health plan outcomes; both operational and financial. Also not surprising was the increasing importance of digital tool access among younger members. With digital platforms playing such a pivotal role in payers’ CX success, generational trends are becoming a particular area of interest for today’s leading payer organizations.
As such, this CX survey report will focus on overlaps and differences across members of certain ages and the CX trends that will help payers position themselves for ongoing wins in member engagement with members of all ages.

Research Scope and Approach
About the Survey
In April of 2022, Zipari and Ipsos launched an online survey to health plan members and health plan representatives. The survey asked members and payers to use a five-point scale to rate their level of satisfaction with different components of their member experience (CX), including through a member portal or mobile app. Other questions asked respondents to select from a menu of responses about health plan frustrations and preferences, including N/A or ‘Other’ to avoid forcing respondents into choices that did not accurately reflect their perspectives or experiences.
The survey included 35 foundational questions, although through branching logic, different respondents answered only those survey items that were applicable to their circumstances. Responses were stratified by market segment, rurality, age group, overall satisfaction with health plan, frequency of health plan contact, and access to digital CX. In general, response patterns did not differ significantly by gender or rurality, but in many instances, did differ by generation, and by status of digital access.
About the Respondents
Member respondents (3,003) were adults ages 26 and older enrolled in employer-sponsored health insurance (32%), individual (15%), Medicare (36%), Medicaid (14%) and military-sponsored health insurance (3%). Twenty-eight percent of the respondents were of the millennial generation, 30% GenX, and 42% baby boomer. These proportions were about the same as in the population of respondents in our 2021 survey. About equal proportions of each age group were male and female. Race and ethnicity distributions were aligned with the US Census and 46% of the member respondents were from suburban areas while 29% and 25% were from urban and rural areas respectively. Thirty-nine percent were employed full time and 30% were retired, about half were married and about 60% had completed at least some college. Two percent of the sample completed the survey in Spanish.
Payer respondents (400) were from small (73%) and large (27%) payer organizations. Seventy-eight percent held mid-level positions, and 76% were managers or above. Fifty-six percent offered employer-sponsored health plans, 55% offered individual plans, and 94% offered government-sponsored plans, like Medicaid and Medicare. Most payers served members in a combination of rural, suburban, and/or urban areas, and 2% completed the survey in Spanish.
What’s New In 2022
Last year’s survey data showed the increasing importance of digital to younger generations. So this year, it wasn’t surprising to see the increasing proportion of millennials and even GenXers who endorsed a preference for app/push notifications and text messaging as communication channels, even while fewer boomers endorsed each of these channels than they did in 2021. Age is becoming an increasingly important factor that payers must consider in their member engagement work.
The 2022 survey included a new question about chatbot communication, and one in five millennials endorsed chatbots as preferred channels for health plan communication. While endorsement was lower for GenXers and boomers, this new data point gives clear direction to health plans whose memberships include ever-growing proportions of members from younger generations.
What About the Call Center?
And what about the call center? Last year we made an assertion about the call center that may have seemed surprising coming from a tech company. We predicted that the call center is here to stay and that digital tools should be used to optimize, not replace, this critical heart of the health plan. This year’s data only strengthens the case with more members endorsing the call center over every other communication channel. In 2022, 45% of the full sample endorsed preferring to communicate with their health plan through the call center; an increase over the 43% who endorsed this option in 2021.
The call center was the top choice for every generation, with slight but consistent increases by millennials, GenXers, and boomers alike.
Prefers The Call Center
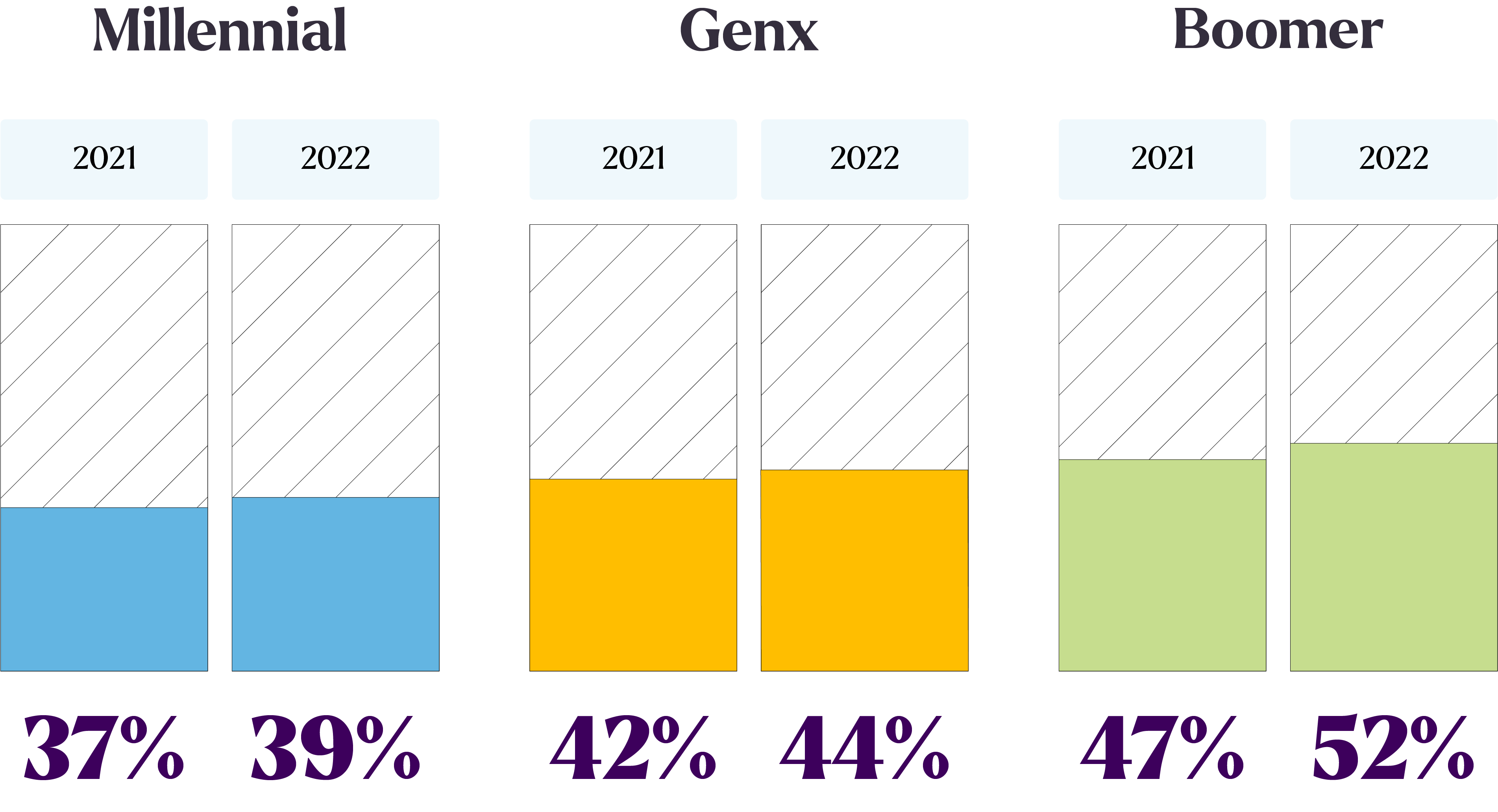
To be frank, we were pretty surprised by these findings last year and wanted to find out more. So, our 2022 survey included a new follow-up question asking respondents about what most influences their choice about how to contact their health plan. By far, the most popular response was, “I prefer to talk to a real person,” endorsed by 60% of the full sample. While this was driven in large part by boomers (three-quarters of whom wanted to talk to a real person) it was also endorsed by high numbers of all generations. Over half of GenXers, and most surprisingly, almost half of millennial respondents agreed.
Prefers to Talk to a Real Person

A small percentage of the overall sample (12%) noted that they preferred calling in because their issues were too complicated to address with digital tools. Interestingly, the largest number of those members were millennials (44%) as compared to 30% and only 25% of GenXers and boomers respectively. Only 8% of the full sample indicated that they could not use digital tools because they lacked internet access, but also surprisingly, over half of those in this category were millennials.
Respondents who noted preferences for digital tools ranked the speed and convenience of these communication channels about equally. About a third of respondents chose each of these options, and as anticipated,the speed and convenience of digital tools was endorsed by more millennials than GenXers, and more GenXers than boomers.
Respondents could choose as many options as were applicable for them on this item, and these response patterns support last year’s finding that the majority of members want multiple communication options. They want to talk to a real person about some issues but want the speed and convenience of digital tools to quickly address more basic tasks. Zipari recently collaborated with Fierce Health Payer on a white paper describing some key facts health payers should know about consumer experience. This paper included highlights from interviews with some health plan leaders. Respondents were given a chance to provide any additional details about what influences their communication choices and 42 members responded. The most frequent response was consistent with the theme of situationally-dependent preferences, as aptly summarized here: “depends on WHY I am contacting them – I can use all these over the course of a year.”
Communication Frustrations
Echoing last year’s findings, almost half of members (46%) do not experience frustrations communicating with their health plan. But, that still leaves a majority who do. Having 54% of members still express frustration with basic health plan communication limits member satisfaction and loyalty potential – but also creates an opportunity to make basic health plan improvements and gain important market advantages. Adding strength to the important narrative about the call center – contacting customer service persists as this year’s greatest frustration across all generations. Of those members who do experience communication frustrations, 32% found customer service interactions the most frustrating, and this was almost 40% within the subset of boomer respondents. Sixty-two members chose to provide free-response details related to their frustrations. These responses were a continuation on the theme with the greatest number noting frustrations with the automated phone system, followed closely by the number frustrated with the long wait times on calls, and some members who noted both. For example: What do you currently find most frustrating about communicating with your health insurance plan? “Long wait times and onerous phone connection menus when calling to get a knowledgeable rep.”
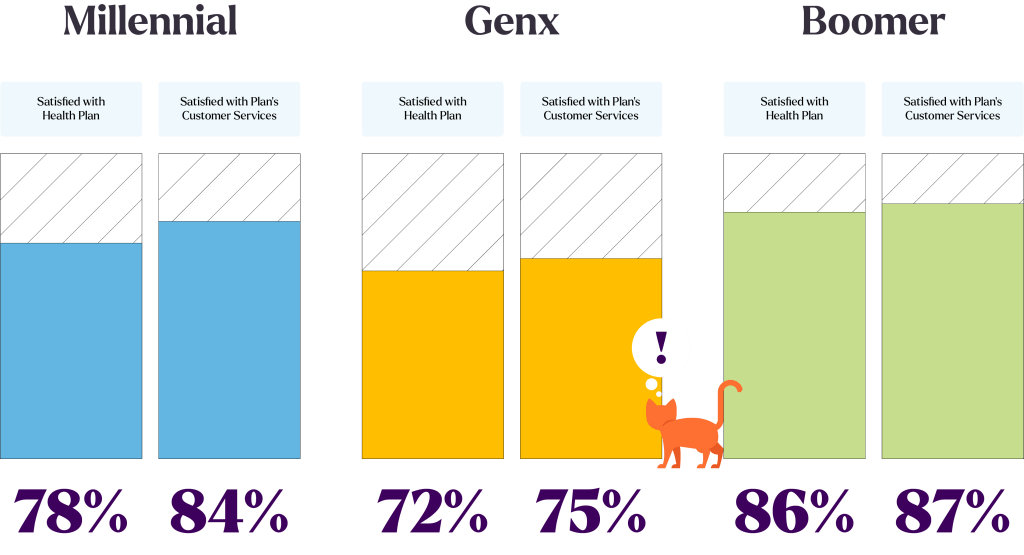
Satisfaction is Booming
Despite some persistent health plan frustrations, rates of satisfaction continue to soar. Across the full member sample, 80% were satisfied with their health plan, and 82% were satisfied with their plan’s customer service. While this is positive news, it’s important for payers to realize that these scores are driven largely by boomers! Close to 90% of boomers are happy with their health plan and their plan’s customer service (86% and 87% respectively), and over half of them are very satisfied. Rates of satisfaction are not quite as high for millennial and GenX populations. Interestingly, while we have thus far seen consistent generational patterns of GenXers falling between millennials and boomers in opinions and expectations as well as age, satisfaction trends are different. Millennials and boomers show higher rates of satisfaction with their plan and customer service experiences, with GenX providing payers with the greatest opportunities for improvement.
What do you currently find most frustrating about communicating with your health insurance plan? “Long wait times and onerous phone connection menus when calling to get a knowledgeable rep.”
Zipari Insight

We predicted that the service center will remain at the heart of health insurance, and we now have two years of data that support that prediction. As a health-tech company, Zipari is of course, a strong advocate for digital tools and self-service opportunity. We work with health plans every day and based on this direct experience, and our market research with members and payers, we know the strong ROI potential these digital tools bring to plans. But, we also know that these tools must be part of a sound CX strategy that recognizes the key role of the service center and the importance of service center representatives to effective member engagement and member satisfaction.
A recent Gartner publication highlights some of the challenges health plans face in providing a unified service experience after implementing multichannel CX. Gartner stresses the importance of creating a seamless member experience across assisted and self-service channels, and knows that service center agents are the foundation of this CX success. Gartner’s recommendations include empowering agents with the right training and resources, and ensuring that experienced service agents are included as the health plan develops service processes and workflows using a unified agent desktop. Health plans who see the wisdom in these recommendations but want to move forward efficiently, should consider an industry-specific tech partner.
By leveraging not just CX expertise, but health-insurance specific CX expertise, plans gain solutions that are already designed to create seamless member experiences across new and legacy technology. And, most importantly, they gain support in implementing these solutions within a thoughtful and orchestrated CX strategy. The right health-plan tech partner will offer effective strategic insights and help you tailor these for your unique plan and member population.
Key Takeaways

In summary, the service center still remains at the heart of health insurance for members of all ages and must remain a key focus for health plans looking to provide a winning member experience and ease member frustrations. Long holds and onerous automated phone systems are not cutting it.
In addition, digital self-service is becoming increasingly important to younger members, and age-related differences in expectations and health plan satisfaction are only expanding. Health plans who have been lulled into CX complacency by relatively high member satisfaction ratings should be careful: these positive ratings are driven largely by baby boomers, the generation that will make up an ever smaller proportion of health plan membership over time. Meanwhile, GenX members are less satisfied than their younger and older peers.
Health plans who can orchestrate a coordinated experience for these members, offering them different opportunities for engagement that align with varying needs and goals, have an opportunity to gain competitive advantages in member loyalty and improved health care utilization.
How can breakthrough CX help your health plan?
Learn how by scheduling a demo today.
